By Aeruxo � Licensed flight dispatcher (study guide) | 15+ Years in Airline Operations
The ACARS message appeared on my screen at 22:47: “PAX MEDICAL EMERGENCY. CPR IN PROGRESS. REQUEST NEAREST SUITABLE.”
Twelve words. No context. No diagnosis. No time for questions. A passenger on our Incheon-to-Manila flight was in cardiac arrest somewhere over the South China Sea, and the cabin crew was performing CPR while the Captain waited for me to tell him where to land.
I had approximately four minutes to identify the nearest airport with adequate medical facilities, verify weather conditions, confirm the runway could handle our aircraft, calculate whether the fuel was sufficient, and send the crew a recommended diversion plan. Four minutes. A person’s life might depend on how quickly and accurately I did my job.
A medical emergency plane situation is the scenario where the dispatcher’s role shifts from planning to crisis management in the sharpest possible way. Every other type of disruption I handle�typhoons, winter storms, engine issues�allows at least some time for analysis. Medical emergencies do not. Someone’s health is deteriorating at 35,000 feet, in a pressurized tube with no hospital, limited medical equipment, and no way to bring help to the patient. The only option is to bring the patient to help. And that means getting the aircraft on the ground, fast.
This article is the story of how that happens�from the perspective of the person on the ground who makes it possible.

Key Takeaways
- In-flight medical emergencies occur on roughly 1 in 600 commercial flights. They are not rare events�they are a regular operational reality that dispatchers and crews prepare for on every flight.
- The dispatcher’s response time is measured in minutes. When a medical diversion is requested, the dispatcher must identify and recommend a diversion airport within 3-5 minutes.
- Not all airports are equal for medical diversions. The nearest airport geographically may not be the best choice if it lacks a hospital, has a short runway, or is closed at night. The dispatcher must evaluate medical capability, operational suitability, and accessibility simultaneously.
- Airlines use ground-based medical consultation services (like MedLink or STAT-MD) that connect the crew with emergency physicians via satellite phone, providing real-time medical guidance to help decide whether a diversion is necessary.
- Medical diversions on Southeast Asian routes present unique challenges because hospital quality, airport facilities, and immigration procedures vary enormously across the region.
This article is based on real operational experience managing in-flight emergencies in an airline Operations Control Center (OCC), where time-critical decisions directly impact passenger safety.
1. How Common Are Medical Emergencies on Planes?
More common than you might think. According to a 2025 study published in JAMA Network Open�the largest study of in-flight medical emergencies ever conducted�approximately 1 in 600 commercial flights involves a medical event significant enough to require crew intervention.
On our network of short-to-medium haul flights across Japan and Southeast Asia�flights of 3-6 hours with 180+ passengers�I encounter medical events regularly. Not daily, but several times per month across all flights on my desk. The vast majority are minor: fainting, nausea, anxiety attacks, or passengers with pre-existing conditions that flare up during flight. These are managed by the cabin crew with the onboard first aid kit and do not require a diversion.
But a meaningful percentage�roughly 7-10% of reported in-flight medical events�are serious enough to warrant consideration of a diversion. And a smaller subset are genuine life-threatening emergencies where the speed of the response directly impacts the patient’s outcome.
The most common serious in-flight medical events I have dealt with include suspected cardiac events (chest pain, cardiac arrest), severe allergic reactions (anaphylaxis), loss of consciousness of unknown cause, seizures, and diabetic emergencies. Each requires a rapid, coordinated response from the cabin crew, the flight deck, the ground-based medical consultation service, and me.
2. “What Happens During a Medical Emergency Plane Response”
Before I even know about the medical emergency, the cabin crew has already begun their response. Commercial cabin crew are trained in emergency first aid, CPR, and the use of automated external defibrillators (AEDs). Their immediate actions follow a well-practiced protocol:
Assess the patient. Is the passenger conscious? Breathing? Responsive? The cabin crew performs a rapid assessment and begins basic life support if needed�clearing the airway, positioning the patient, starting CPR if there is no pulse.
Retrieve the emergency medical kit. Every commercial aircraft carries an emergency medical kit (EMK) containing medications, a stethoscope, blood pressure cuff, IV supplies, and other tools that a qualified medical professional can use. The crew also has access to an AED�an automated defibrillator that can be used by trained non-medical personnel to treat cardiac arrest.
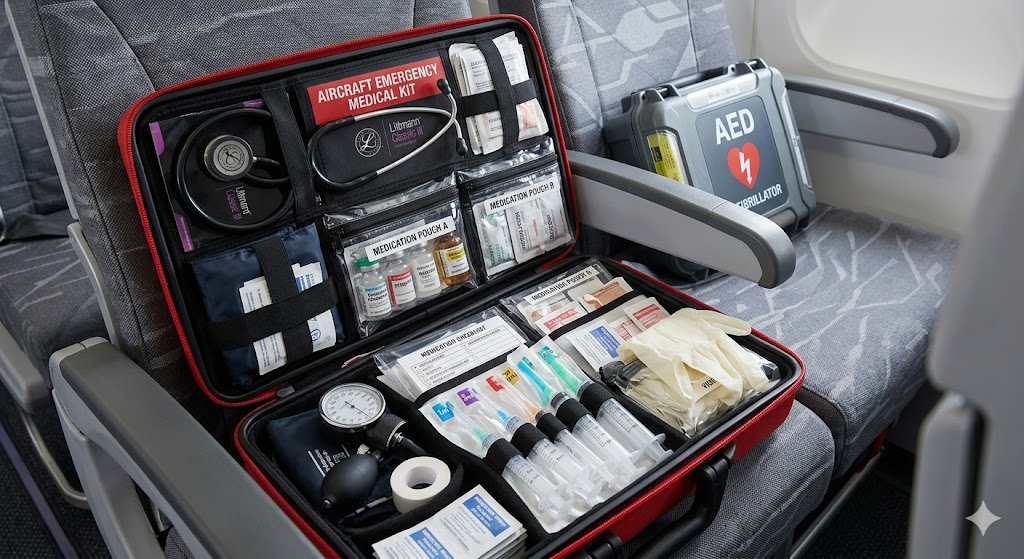
Call for medical volunteers. The PA announcement that many passengers dread: “If there are any medical professionals on board, please identify yourself to a crew member.” This call reaches doctors, nurses, paramedics, and other healthcare professionals who may be traveling as passengers. On a flight with 180+ passengers, the probability of having at least one medical professional on board is surprisingly high�studies suggest roughly 50-70% of flights have a physician or nurse among the passengers.
Notify the flight deck. The senior cabin crew member contacts the Captain to report the situation. This is the moment the cockpit and the OCC become involved.
3. The Dispatcher’s Response: 4 Minutes That Matter

The moment the Captain decides a medical diversion may be necessary, the clock starts for me. Here is the exact sequence of actions I perform, typically in under 5 minutes:
Minute 1: Identify the Aircraft Position and Nearest Airports
I pull up the aircraft’s current position on the flight tracking display. I overlay nearby airports and rapidly assess which ones are viable diversion candidates. “Nearest” is not always “best”�I am filtering for multiple criteria simultaneously:
Runway suitability: Can our aircraft type land there? Is the runway long enough? Is it equipped for our approach category? A regional airport with a 1,500-meter runway will not work for a fully loaded 737-800 that needs 2,000+ meters.
Operating hours: Is the airport open? Many smaller airports in Southeast Asia close at night. If it is midnight local time and the nearest airport closes at 22:00, it is not an option unless I can arrange an emergency opening�which takes time we may not have.
Medical facilities: This is the critical differentiator for medical diversions. The nearest airport might be a small regional field with no hospital within 30 minutes. The second-nearest might be a city with a major medical center 10 minutes from the airport. For a cardiac arrest, those 20 extra minutes of hospital access time could be the difference between life and death.
Minute 2: Check Weather and Verify Fuel
I pull the latest METAR for the candidate diversion airports. Weather that is acceptable for a routine arrival might not be suitable during a time-critical diversion�I need airports where the crew can make a straight-in approach without holding or complex maneuvering. I also verify fuel: does the aircraft have enough fuel to reach the diversion airport with required reserves? On our routes, the answer is almost always yes, because I build diversion fuel into every flight plan.
Minute 3: Coordinate with Ground Medical Support
Most airlines subscribe to a ground-based medical consultation service�companies like MedLink (operated by MedAire) or STAT-MD that employ emergency physicians who are available 24/7 via satellite phone. The flight crew connects with these physicians, who provide real-time medical guidance: what medications to administer from the EMK, what procedures to perform, and critically, whether a diversion is medically necessary or whether the patient can be stabilized for continued flight to the destination.
While the crew is consulting with the ground medical service, I am preparing the diversion plan so that if the decision is “divert,” we can execute immediately without additional delay.
Minute 4: Send the Recommendation and Coordinate
I send an ACARS message to the crew with my recommended diversion airport, the weather conditions, the expected approach type, and any relevant information about ground facilities. Simultaneously, I begin coordinating with the diversion airport: alerting the ground handling agent (if we have one), requesting an ambulance to meet the aircraft, and notifying the airport authority of our inbound medical diversion.
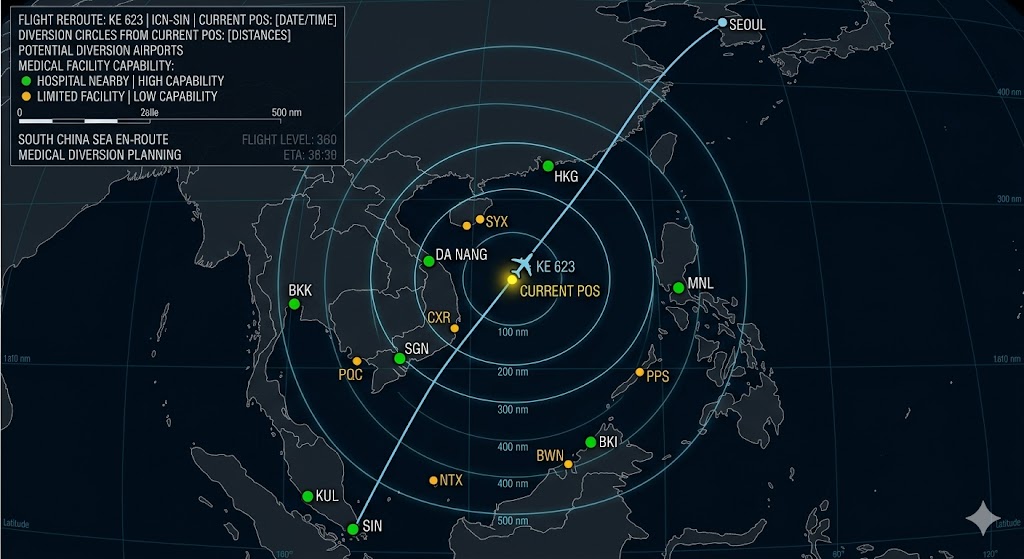
The entire sequence�from receiving the initial ACARS message to sending the diversion recommendation�takes 3-5 minutes. In a genuine cardiac arrest, every one of those minutes matters. This is why I maintain a mental database of airports along our common routes, including their medical facility proximity and quality. When the message comes in, I am not starting from zero�I am recalling information I have already processed and verified during flight planning.
4. The Diversion Decision: Who Decides, and How
The decision to divert for a medical emergency is ultimately the Captain’s. But it is informed by multiple inputs:
The ground medical physician’s assessment: Is this condition life-threatening? Will delay in reaching a hospital materially affect the outcome? Can the patient be stabilized with onboard resources?
The volunteer medical professional’s assessment (if available): A doctor on board provides hands-on evaluation that the ground physician cannot. Their recommendation carries significant weight.
The dispatcher’s operational assessment: Is the diversion operationally feasible? What are the consequences for the aircraft, crew, and remaining passengers?
The Captain’s judgment: The Captain weighs all inputs and makes the final call. In my experience, Captains almost always err on the side of diversion when there is genuine uncertainty about a patient’s condition. The potential consequences of not diverting (a death on board) are catastrophic; the consequences of an unnecessary diversion (delay and cost) are manageable.
I support this bias toward diversion completely. As I wrote in my article on aviation safety, the system prioritizes safety above schedule, always. In the context of a medical emergency, “safety” means getting a sick passenger to a hospital as quickly as possible.
5. Medical Diversions on Southeast Asian Routes: Unique Challenges
Medical diversions on our Japan and Southeast Asian network present challenges that do not exist on domestic routes or flights within well-developed aviation infrastructure.
Hospital quality varies dramatically. A diversion to Manila or Bangkok puts the patient within reach of world-class hospitals. A diversion to a smaller regional airport in Vietnam or the Philippines may mean a hospital with limited emergency capabilities, no cardiac catheterization lab, and potentially no English-speaking staff. I factor this into my airport selection�sometimes the “nearest” airport is not the best choice for the patient.
Immigration complications. If a flight from Incheon to Denpasar diverts to an airport in a different country�say, Ho Chi Minh City in Vietnam�the passenger may not have a Vietnamese visa. Immigration authorities must be contacted in advance to arrange emergency entry for the patient. This adds coordination time but is generally managed smoothly because immigration services at international airports are accustomed to medical diversion scenarios.
Ground handling at non-regular destinations. As I described in my article on flight diversions, our LCC may have no ground handling presence at a diversion airport. I have coordinated medical diversions to airports where I had to call the airport authority directly to arrange ambulance access to the aircraft�at 2 AM, with limited English communication, while simultaneously managing the cockpit crew’s needs and the remaining passengers’ situation.

Language barriers. On flights carrying predominantly Korean passengers with a medical emergency diverting to a non-Korean-speaking country, communication between the patient and local medical personnel becomes an additional challenge. The cabin crew often serves as interpreters during the handoff to local paramedics�another layer of complexity in an already demanding situation.
6. What Happens After the Patient Is Off the Aircraft
Once the patient has been offloaded and transferred to local medical services, the operational challenge shifts to recovery.

Can the flight continue? In most medical diversion cases, the flight can resume to the original destination after the patient is offloaded. The ground stop typically takes 1-2 hours�time for refueling (if needed), a crew assessment of remaining duty time, and passenger reseating. The remaining passengers continue to their destination, delayed but safe.
Crew duty time check. The diversion has added time to the crew’s duty day. I must verify that the crew can still legally complete the flight to the destination and, potentially, the return flight. If the crew will exceed their duty limits, the flight either waits for a crew rest period or I arrange a replacement crew�which, at an LCC outstation, may not be available until the next day.
The patient’s companion. If the patient was traveling with family or friends, they are typically offloaded with the patient. Their luggage must be retrieved from the cargo hold�which requires opening the hold and potentially reorganizing cargo, adding time to the ground stop.
Cascading schedule impact. The 1-2 hour diversion delay cascades through the aircraft’s remaining schedule for the day. Subsequent flights on this aircraft are delayed. If the delay pushes later flights past crew duty limits, cancellations may follow. A single medical diversion on the morning’s first flight can disrupt the entire day’s schedule across multiple routes.
7. The Scenarios That Keep Me Alert
After 15 years, certain medical emergency scenarios have taught me the most about the importance of preparation and speed.
The cardiac arrest over the South China Sea. The scenario I described at the opening of this article. The aircraft was equidistant between Da Nang and Manila�roughly 90 minutes from each. Da Nang was slightly closer and had a hospital 15 minutes from the airport. Manila was further but had superior cardiac care facilities. The ground medical physician recommended the nearest hospital. I sent Da Nang. The aircraft diverted, landed 75 minutes later, and the passenger was transferred to the hospital. I later learned the passenger survived.
The allergic reaction at midnight. A passenger on a late-night flight experienced anaphylaxis�a severe allergic reaction that causes airway swelling and can be fatal within minutes. The cabin crew administered epinephrine from the emergency medical kit, which stabilized the patient, but the ground physician recommended diversion for hospital observation. The nearest airport was a small regional field in the Philippines that was closed for the night. The next option was Clark International�40 minutes further but open 24 hours with hospital access. I recommended Clark. We arrived, the patient was transferred, and made a full recovery.
The decision not to divert. Not every medical event requires a diversion, and the dispatcher’s role includes supporting the decision to continue when that is the right call. A passenger experienced a fainting episode two hours from the destination. A nurse on board assessed the patient, found stable vital signs, and attributed the episode to dehydration and anxiety. The ground physician concurred. The Captain decided to continue to the destination, where the passenger was met by airport medical staff on arrival. No diversion was needed, and 180 other passengers arrived on time. Knowing when not to divert is as important as knowing when to divert.
8. What Passengers Can Do
As someone who has managed the operational side of dozens of medical diversions, here is my practical advice for passengers:
Carry your medications in your carry-on, not your checked bag. If you have a chronic condition�heart disease, diabetes, severe allergies�your medications should be within arm’s reach, not in the cargo hold. In a medical emergency, the cabin crew will ask about your medications. Having them immediately accessible speeds up treatment.
Carry a health summary card. A card listing your medical conditions, medications, allergies, and emergency contacts can be invaluable if you are unable to communicate during a medical event. The cabin crew can relay this information to the ground medical physician, significantly improving the quality of remote medical guidance.
Stay hydrated and move during long flights. Many in-flight medical events�fainting, dizziness, deep vein thrombosis�are exacerbated by dehydration and prolonged immobility. Drink water regularly and move your legs periodically. These are simple precautions that meaningfully reduce your risk.
If you are a medical professional, please respond. I know it is your day off. I know you are traveling for vacation, not work. But when the PA asks for medical volunteers, your expertise can make an extraordinary difference. The cabin crew are trained in first aid, but they are not physicians. A doctor’s assessment�even a brief one�provides critical information that helps the crew, the ground medical service, and me make better decisions about whether to divert. You may save a life by giving 20 minutes of your time.
If you feel unwell, tell the crew early. Do not wait until you are losing consciousness to seek help. Early intervention is always more effective than crisis management. The cabin crew would far rather check your blood pressure when you first feel dizzy than perform CPR after you collapse in the aisle.
9. The Weight of the Decision
I want to end with something personal. Medical diversions are the decisions that stay with me longest. Not because they are the most operationally complex�typhoons are more complex, winter operations are more grinding. But because medical diversions are the only decisions where a human life hangs in the balance in an immediate, personal way.
When I select Da Nang over Manila for a cardiac arrest patient, I am making a judgment call that directly affects whether that person lives or dies. If I choose wrong�if Da Nang’s hospital does not have the capability to treat the specific condition, or if the 20 extra minutes to Manila would have provided access to a cardiac catheterization lab that saved their life�that is a consequence I have to live with.
I have never made a medical diversion decision that I regret. But I have made decisions where I did not know the outcome�where the patient was transferred to a local hospital and I never learned what happened next. Those are the ones that occupy my thoughts during quiet moments on the night shift.
What I do know is this: every medical diversion I have coordinated resulted in the patient reaching medical care faster than they would have if we had continued to the destination. That is the purpose of the system. That is what flight crews and dispatchers are trained to do. And in the moments that matter most�when someone’s life depends on how quickly we can get an airplane on the ground�the system works.
Learn more about our mission and operational background on the About Aeruxo page.
Frequently Asked Questions
How often do medical emergencies happen on planes?
According to the largest study on the topic (JAMA Network Open, 2025), approximately 1 in 600 commercial flights involves a medical event requiring crew intervention. The most common incidents are fainting, nausea, and respiratory symptoms. Serious events requiring diversion occur less frequently�roughly 7-10% of reported medical events, or approximately 1 in 6,000-8,000 flights.
What medical equipment is on a commercial airplane?
All commercial aircraft carry first aid kits (containing bandages, basic medications, and supplies), an emergency medical kit (containing more advanced medications, IV supplies, a stethoscope, and blood pressure cuff), and an automated external defibrillator (AED). The exact contents are regulated by aviation authorities and vary somewhat by country. These supplies are designed to stabilize a patient until they can reach a hospital�not to provide definitive treatment.
Does the airline have to divert for a medical emergency?
There is no universal regulatory mandate requiring diversion for every medical event. The decision is made by the Captain based on input from the ground medical service, any volunteer medical professionals on board, and the flight dispatcher. Diversion is recommended when the patient’s condition is assessed as potentially life-threatening and delay in reaching hospital care could worsen the outcome. For non-life-threatening conditions that can be managed with onboard resources, the flight typically continues to its destination.
Who pays for a medical diversion?
The airline bears the direct costs of the diversion (landing fees, fuel, ground handling, schedule disruption). The patient is generally not charged for the diversion itself. However, the patient is typically responsible for their own medical treatment costs at the diversion hospital�which is why travel health insurance is essential, especially for international travel. Some travel insurance policies specifically cover medical evacuation and treatment costs abroad.
Can I refuse to let the plane divert for me?
A patient can express a preference, but the Captain has final authority over the aircraft and can overrule a patient’s wishes if the medical situation warrants it. In practice, if a ground medical physician and a volunteer doctor both recommend diversion for a serious condition, the Captain will divert regardless of the patient’s preference. The Captain’s legal responsibility for the safety of everyone on board takes precedence.
What should I do if I have a medical condition and want to fly?
Consult your physician before traveling, especially if you have cardiac, respiratory, or other conditions that could be affected by altitude and cabin pressure. Carry all medications in your carry-on with a doctor’s note. Consider a health summary card listing your conditions, medications, and allergies. Stay hydrated during the flight and move periodically. Inform the cabin crew of any condition that might require attention during the flight�they would rather be prepared in advance than surprised by an emergency.
Have you experienced or witnessed a medical emergency on a flight? Share your story in the comments�I am especially interested in the passenger perspective of these events.
Disclaimer: The views expressed in this article are my own professional opinions based on 15+ years of operational experience. They do not represent the official position of any airline, aviation authority, or regulatory body. All patient details have been generalized to protect privacy.

Licensed Flight Dispatcher with 15+ years of experience in airline operations control. Holds FAA Aircraft Dispatcher Certificate and Republic of Korea Flight Dispatcher License (MOLIT). Specializes in flight watch, NOTAM analysis, flight planning, and operational control at a Korean LCC. IOSA audit participant and author of multiple airline operational manuals, including Emergency Response, De-icing, and OCC Procedures.